
According to Bizfluent, the majority of U.S. hospitals are nonprofit. Their tax-exempt status requires them to provide more community-based health programs and to attend to all patients irrespective of financial status. On the other hand, for-profit hospitals have the ability to stock the latest medical technologies and are well-suited for advanced care. Here is a comparison of both types of hospitals to determine which is better.
Cost
This is where nonprofit hospitals shine. They traditionally charge lower rates than for-profit hospitals for almost all medical procedures. The icing on the cake is that the lower-cost care does not come with a corresponding drop in quality level. Statistics show that despite charging more, for-profit hospitals perform worse than nonprofit hospitals when it comes to treating common illnesses, and, consequentially, have higher death rates. That is because the quality of care depends on the ability of employees and the institution’s general policies.
Accessibility
The federal government requires all hospitals to administer free stabilizing care to all patients who seek help. They are all supposed to save lives and ensure that all patients are out of danger before asking for compensation. For-profit hospitals can lawfully release patients who lack the ability to pay for further treatment after they establish that they are out of danger. Nonprofit hospitals are obligated to treat all conditions, whether life-threatening or not, regardless of the patients’ financial or health insurance status.
Equipment
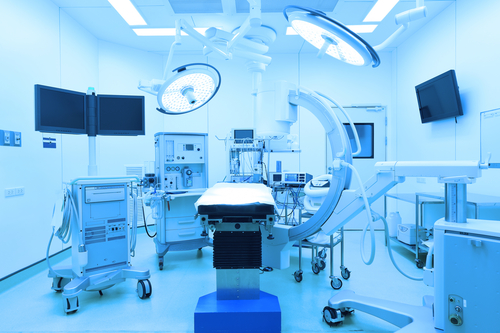
Even with tax exemption, most nonprofit hospitals are struggling financially. They bring in less money than their for-profit counterparts and most have huge debts. On the other hand, for-profit hospitals enjoy financial stability and most are not only debt-free but also able to purchase the needed advanced medical technologies. For-profit hospitals, therefore, are better equipped and provide better surgical services and diagnostic procedures than nonprofit hospitals.
Community Support
Nonprofit hospitals have an obligation to the community. They have a responsibility to provide and promote smaller community health organizations such as free acute-care centers and community health clinics. For-profit hospitals’ responsibility is the investors. They have to accrue enough profit to pay dividends to the shareholders while still taking the enterprise in the approved direction. Their pressure to maximize profits limit their support to the community.
Uncompensated Services
The tax-exempt status comes with a condition: all nonprofit hospitals are to give away a certain amount of their services to the community. These services are known as uncompensated services are a measure of a hospital’s benefit to the community. They include the writing off of bad debts and the provision of charity care. Although the IRS is not very strict on the percentages of uncompensated services, nonprofit hospitals still give away a greater proportion of their services compared to similarly situated for-profit hospitals.
Variety
Nonprofit hospitals offer expensive yet financially-nonviable facilities such as intensive care burn and high-level trauma wards. They also provide services that benefit the community at the expense of the hospitals’ income such as drug treatment programs and psychiatric care. For-profit hospitals invest in facilities for treating expensive conditions including state-of-the-art tech for cardiac or complicated diagnostic services.
Location
Counterintuitively, richer neighborhoods boast more nonprofit hospitals, while high-poverty areas are home to more for-profits. That means that there are more nonprofit hospitals in Northeastern and Midwestern states compared to Southern states. The result is that people who can afford insurance enjoy cheaper services than those who cannot.
Apart from the ability to purchase, equip, and maintain expensive machinery, for-profit hospitals lose to nonprofit hospitals in most frontiers. Nonprofit hospitals are ideal for most illnesses and injuries, but the lack of advanced technology may force some patients to seek specialized care from the more-expensive for-profit facilities.
Pro: Greater Number of Nonprofit Hospitals
In the United States, there are about 5,200 non-federal hospitals, explains Non-Profit Quarterly. About 3,000 of them are nonprofit hospitals. For a person in need of ambulatory surgical care, inpatient surgery or other hospital services, there are more options in the nonprofit sector. It’s important to note that the concentration of nonprofit hospitals varies by geographic location. In general, there are more nonprofit options in the West, Northeast, Southwest and Midwest compared to the South. In Florida, Nevada and Texas, for-profit hospitals account for more than 50% of facilities.
Pro: Community Orientation
While for-profit hospitals have to put their shareholders and investors first, a non-profit institution can put its customers first. When patients are put as the top priority of the hospital, they receive better care. Since earning a profit from each patient isn’t the top priority, a nonprofit facility can put more effort on achieving the best possible outcome for the patient. In some cases, that necessitates a longer stay or an additional test. In other cases, it might require care from more specialists. A patient-centered approach to healthcare typically results in higher patient satisfaction rates with their healthcare services.
Pro: Plan for the Long-term Future
A non-profit hospital is better able to plan for the long-term future. The administrators don’t have to spend as much time worrying about this quarter’s billable amounts or the next quarter’s estimated income. Instead, they can focus on what could make their hospital a better place for patients and staff. They can turn to data in order to hone in on which services should be expanded. For example, type 2 diabetes is becoming more common in children, and a non-profit hospital could add a program for community outreach around this issue.
Pro: More Willing Accept Community Feedback
A non-profit hospital is more likely to ask for and act on feedback from the community. This type of institution sees itself as serving the community, while a for-profit hospital often looks to approval from its investors and shareholders first. If members of the community start to notice a problem, such as emergency room waits that are excessive, the administrators of a non-profit healthcare facility are more likely to take a look at what is causing this issue. At a for-profit hospital, they may only make a change if it is in their best financial interest to do so.
Pro: Wide Range of Services at Non-profit Hospitals
A non-profit hospital is more likely to offer a wide range of services, including services that don’t typically generate a lot of income. For example, neonatal intensive care units are costly to operate. They’re a high risk for a hospital that needs to generate ever-increasing profits. The neonatal intensive care units take care of the sickest and most medically fragile babies, and their costs of care can be astronomical. Some of these babies are hospitalized for months before they’re well enough to go home for the first time. A specialty unit that isn’t profitable but serves the community’s needs is more likely to persist at a non-profit hospital.
Featured Programs
Pro: No Incentive to Bill for Non-essential Services
A non-profit hospital has no incentive to upcharge its patients or bill for non-essential services. There are many anecdotal reports of patients being billed $7 for one aspirin or hundreds of dollars for a basic laboratory test that only costs a couple of dollars to perform. Since the non-profit hospital doesn’t have to worry about making extra money off these areas of patient care, it has no incentive to run up the costs for their patients. Non-profit hospitals may also have more consistent pricing policies for the patients who are self-pay versus those who have public or private insurance.
Pro: Partnership with Community Organizations
When a non-profit hospital finds itself without enough staff to run a program, it can often count on the community for help. Partnerships with community organizations allow non-profit hospitals to do a lot more with the resources they have. In many cases, other nonprofit organizations within the community step up in order to coordinate some of the most popular services. These partnerships allow for more outreach and engagement in low-income communities and with people who speak English as a second language. Some common partnerships between nonprofit community organizations and non-profit hospitals include grief support groups, nutrition education, diabetes education and cancer screenings.
Pro: Fast Response to Community Needs
A non-profit hospital can offer a fast response to the needs of a community. Most non-profit hospitals don’t have to go through a corporate board in order to make a policy change, add a service or extend their reach in the community. With the COVID-19 pandemic, many non-profit hospitals were able to quickly ramp up drive-through testing. In Columbus, OH, the Ohio State University’s Wexner Medical Center provided free COVID-19 care kits to residents of the city. Those care kits included face masks, hand sanitizer, disposable gloves and home cleaning products.
Pro: More Flexibility to Handle Current Community Health Issues

Non-profit hospitals have more flexibility to handle a community’s current health issues. For example, Huntington, West Virginia, has been severely impacted by the opioid crisis, and overdoses are a leading cause of death in the city. Cabell Huntington Hospital has expanded its community outreach, offering education to community members and a free supply of a medication that can be administered by a layperson when a person has overdosed on fentanyl or another opioid drug. Each year, the hospital conducts a community health assessment in order to determine what the area’s current needs are, and it uses the information to prioritize its services.
Pro: More Opportunities for Teaching and Training
Non-profit hospitals are often used as facilities for teaching and training new physicians, specialists, nurse practitioners and ancillary healthcare professionals. These new graduates have the latest knowledge in healthcare and medical research, and they may spot things or identify new problems that older healthcare providers miss. When these new physicians work alongside more experienced healthcare providers, the patient benefits both from the newest knowledge and from the years of experience. For the healthcare providers themselves, training at a non-profit hospital provides them with a wider range of patients, diseases and conditions from which they can learn. This is especially important for rare and unusual conditions.
Con: More Administration and Bureaucracy
In some cases, non-profit hospitals have more administrative hurdles and bureaucracy. While a for-profit hospital can consolidate its billing department, medical records department and other administrative services across all of its locations, a non-profit hospital doesn’t have an incentive to do that. A patient who has an issue with their bill or the care they received may have to jump through a lot of hoops in order to get their issue resolved. The lack of clear policies may confuse patients, especially those who have a low education level and who don’t understand the complicated paperwork and billing processes.
Con: May Not Offer Newest Technology or Specialties
While non-profit hospitals have been adding some income-generating specialties to balance their high-cost services, patients may not find the most modern care or technology at a non-profit hospital. A person who’s looking for their knee surgery to be performed by a robot, which is less invasive, may not find this option at a non-profit hospital. The surgical robots are expensive and require a significant amount of training to use. They also take up a lot of space and are complicated to clean. A non-profit hospital might not have the resources to invest in the newest and fanciest equipment.
Con: Longer Waiting Times for Care
Non-profit hospitals are more likely to attract people who need charity care. These people may not have health insurance. Instead of going to their doctor when they have an illness, they may end up waiting until it’s more serious. They arrive at the non-profit hospital’s emergency room with a raging ear infection or pneumonia. This increases the waiting time for everyone, including those who do have private insurance. It’s not uncommon for the emergency room waiting times to be up to 24 hours at a non-profit hospital in a large city.
Con: If They Lose Too Much Money, They Close
Although a non-profit hospital doesn’t have to spend an inordinate amount of time focusing on every nickel and dime, it can’t operate on huge losses every year. There are times when non-profit hospitals will close because it costs too much to keep them open. In some of these cases, the non-profit hospitals are able to get help from community organizations or other nonprofit organizations. Sometimes, several non-profit hospitals join together and form a network, which allows them to consolidate some of the administrative expenses and take advantage of economies of scale. Keep in mind that for-profit hospitals
Resources:
- Top 20 Master’s in Healthcare Online/Online MBA in Healthcare Administration
- 25 Great Scholarships for Healthcare Management Students
- Top 20 Certification Programs in Healthcare Management
- Can I Work in a Hospital with a Healthcare Management Degree?
- How Are Hospitals Becoming More Eco-friendly?
- How Much Does a Hospital Administrator Make?
- What Jobs Are Available in a Hospital Setting with a Healthcare Management Degree?